Hantavirus Pulmonary Syndrome In California – Symptoms Treatment And Prevention
UPDATE: Your best and first source of info should always be the following:
Calaveras County Public Health Department
Colleen A. Tracy, MPH, Acting Public Health Director
Dean M. Kelaita, MD, Local Health Officer
Phone: (209) 754-6460
Fax: (209) 754-1709
CD Reporting: (209) 754-4691
Office Hours:
8:00am – 5:00pm
Monday thru Friday
Mailing Address | Physical Address |
891 Mountain Ranch Road San Andreas, CA 95249 |
Great info from the CDC on Cleaning up after rodents!
When you begin cleaning, it is important that you do not stir up dust by sweeping or vacuuming up droppings, urine, or nesting materials.
- Wear rubber, latex, or vinyl gloves when cleaning urine and droppings.
- Spray the urine and droppings with a disinfectant or a mixture of bleach and water and let soak 5 minutes. The recommended concentration of bleach solution is 1 part bleach to 10 parts water. When using a commercial disinfectant, following the manufacturer’s instructions on the label for dilution and disinfection time.
- Use a paper towel to pick up the urine and droppings, and dispose of the waste in the garbage.
- After the rodent droppings and urine have been removed, disinfect items that might have been contaminated by rodents or their urine and droppings.
| Clothing, Bedding, Stuffed Animals | Carpets/Furniture | Books, Papers and other Non-washable items |
|---|---|---|
| Launder potentially contaminated bedding, clothing, or stuffed animals with hot water and detergent. Use rubber, latex, vinyl, or nitrile gloves when handling contaminated laundry. Machine-dry laundry on a high setting or hang it to air dry in the sun. Laundry detergent breaks down the virus’s lipid envelope, rendering it harmless. Additionally, heat generated by the clothes dryer will also ensure that the virus is noninfectious. However, the use of a clothes dryer alone is not recommended as the sole treatment because not all dryers reach the necessary temperature. A temperature of 45 degrees Celsius, or about 115 degrees Fahrenheit, is required to inactivate hantaviruses. | Shampoo rugs and upholstered furniture with a commercial disinfectant or with a commercial-grade steam cleaner or shampoo. | You may leave books, papers, and other items that cannot be cleaned with a liquid disinfectant or thrown away, outdoors in the sunlight for several hours, or in an indoor area free of rodents for approximately 1 week before cleanup. After that time, the virus should no longer be infectious. Wear rubber, latex, vinyl, or nitrile gloves and wipe the items with a cloth moistened with disinfectant. Once excreted into the environment by the rodent, hantaviruses can survive in the environment and remain infectious for a period of 2-3 days. Ultraviolet rays in sunlight inactivate hantaviruses. |
—————END UPDATE———————
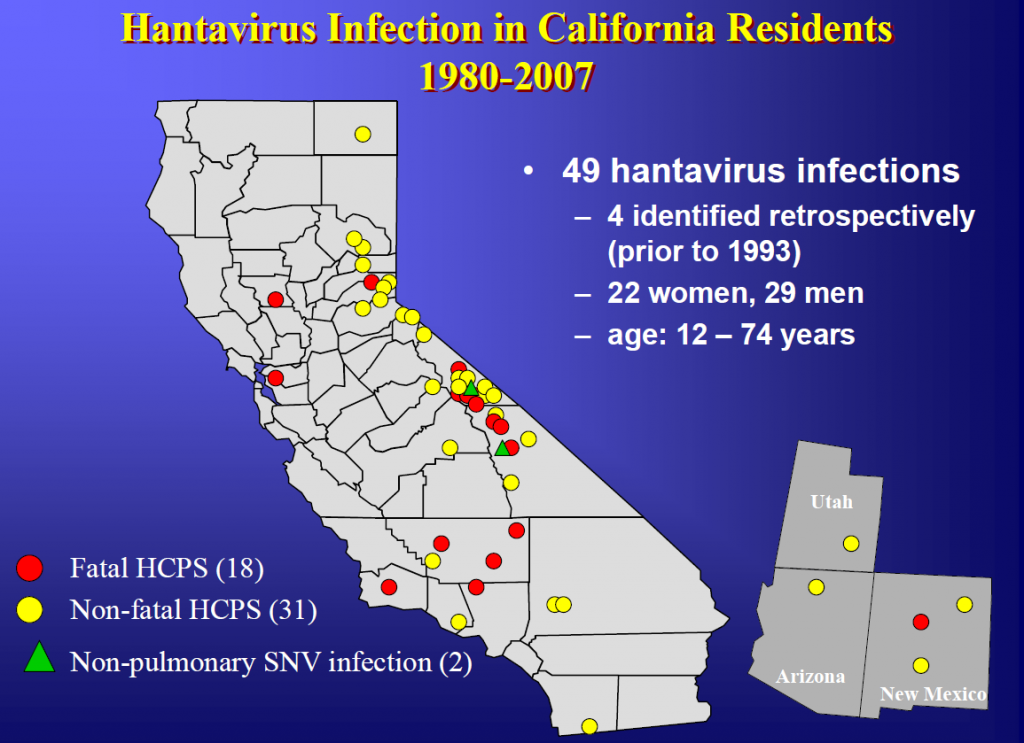
Since HPS was first identified in 1993, there have been 60 cases in California and 587 cases nationally. About one third of HPS cases identified in California were fatal. The two recent cases bring the total California case count for 2012 to four. Case-patients have been exposed to hantavirus in many areas in California where deer mice live, particularly from the eastern Sierra Nevada region and at higher elevations.
Per Wikipedia:
Hantaviruses are negative sense RNA viruses in the Bunyaviridae family. Humans may be infected with hantaviruses through rodent bites, urine, saliva or contact with rodent waste products. Some hantaviruses cause potentially fatal diseases in humans, hemorrhagic fever with renal syndrome (HFRS) and hantavirus pulmonary syndrome (HPS), but others have not been associated with human disease. Human infections of hantaviruses have almost entirely been linked to human contact with rodent excrement, but recent human-to-human transmission has been reported with the Andes virus in South America. The name hantavirus is derived from the Hantan River area in South Korea, which provided the founding member of the group: Hantaan virus (HTNV), isolated in the late 1970s by Ho-Wang Lee and colleagues.HTNV is one of several hantaviruses that cause HFRS, formerly known as Korean hemorrhagic fever.
In 1993, an outbreak of Hantavirus pulmonary syndrome (HPS, see below) occurred in the Four Corners (southwestern corner of Colorado, northwestern corner of New Mexico, northeastern corner of Arizona and southeastern corner of Utah) region in the southwestern United States. The viral cause of the disease was found only weeks later and was called the Sin Nombre virus (SNV, in Spanish, “Virus sin nombre”, for “nameless virus”). Its rodent host, Peromyscus maniculatus, was first identified by Terry Yates, a professor at the University of New Mexico. In addition to Hantaan virus and Sin Nombre virus, several other hantaviruses have been implicated as etiologic agents for either HFRS or HPS. Other identified hantaviruses have not been associated with disease.
Symptoms
Hemorrhagic fever with renal syndrome
Hantavirus has an incubation time of two to four weeks in humans before symptoms of infection occur. The symptoms of HFRS can be split into five phases:
Febrile phase: Symptoms include fever, chills, sweaty palms, diarrhea, malaise, headaches, nausea, abdominal and back pain, respiratory problems such as the ones common in the influenza virus, as well as gastro-intestinal problems. These symptoms normally occur for three to seven days and arise about two to three weeks after exposure.
Hypotensive phase: This occurs when the blood platelet levels drop and symptoms can lead to tachycardia and hypoxemia. This phase can last for 2 days.
Oliguric phase: This phase lasts for three to seven days and is characterised by the onset of renal failure and proteinuria occurs.
Diuretic phase: This is characterized by diuresis of three to six litres per day, which can last for a couple of days up to weeks.
Convalescent phase: This is normally when recovery occurs and symptoms begin to improve.Formerly known as Korean hemorrhagic fever, HFRS is the term accepted by the World Health Organization.
Persons first develop symptoms one to two weeks after exposure to SNV. Early symptoms of HCPS include fever, headache, and muscle aches, especially the thighs, hips, back, and shoulders. Other early symptoms include dizziness, chills, nausea, vomiting, diarrhea, and abdominal pain. After two to seven days of these symptoms,
patients develop breathing difficulties that range from cough and shortness of breath to severe respiratory failure. Approximately 40 percent of HCPS patients die from the disease.Hantavirus (cardio-)pulmonary syndrome
Hantavirus pulmonary syndrome (HPS) is an often fatal disease caused by hantavirus infection. The symptoms are very similar to those of HFRS and include tachycardia and tachypnea. Additionally, patients will develop difficulty breathing, coughing and shortness of breath. Such conditions can lead to a cardiopulmonary phase, where cardiovascular shock can occur, and hospitalization of the patient is required. HPS was first recognized in 1993 in the southwest of the United States by Bruce Tempest MD, and was originally called “Four Corners disease”. It has since been identified throughout the United States. Although rare, HPS is fatal in up to 60% of cases. Rodent control in and around the home remains the primary strategy for preventing hantavirus infection. People suspecting illness are encouraged to contact their local health department.
Treatment
There is no specific treatment, cure, or vaccine for hantavirus infection. However, we do know that if infected individuals are recognized early and receive medical care in an intensive care unit, they may do better. In intensive care, patients are intubated and given oxygen therapy to help them through the period of severe respiratory distress.
The earlier the patient is brought in to intensive care, the better. If a patient is experiencing full distress, it is less likely the treatment will be effective.
Therefore, if you have been around rodents and have symptoms of fever, deep muscle aches, and severe shortness of breath, see your doctor immediately. Be sure to tell your doctor that you have been around rodents—this will alert your physician to look closely for any rodent-carried disease, such as HPS.
HPS is caused by a virus that individuals get through contact with the urine, droppings or saliva of infected wild mice, primarily deer mice. Breathing small particles of mouse urine or droppings that have been stirred up into the air is the most common means of acquiring infection. The illness starts one to six weeks after exposure with fever, headache, and muscle ache, and progresses rapidly to severe difficulty in breathing and, in some cases, death.
Prevention
When you are in wilderness areas or places that harbor mice, you can take the following steps to prevent HPS:
- Avoid areas, especially indoors, where wild rodents are likely to have been present.
- Keep food in tightly sealed containers and store away from rodents.
- Keep rodents out of buildings by removing stacked wood, rubbish piles, and discarded junk from around homes and sealing any holes where rodents could enter.
- If you can clean your sleeping or living area, open windows to air out the areas for at least two hours before entering. Take care not to stir up dust. Wear plastic gloves and spray areas contaminated with rodent droppings and urine with a 10% bleach solution or other household disinfectants and wait at least 15 minutes before cleaning the area. Place the waste in double plastic bags, each tightly sealed, and discard in the trash. Wash hands thoroughly afterward.
- Do not touch or handle live rodents and wear gloves when handling dead rodents. Spray dead rodents with a disinfectant and dispose of in the same way as droppings. Wash hands thoroughly after handling dead rodents.
- If there are large numbers of rodents in a home or other buildings, contact a pest control service to remove them.
- Do not use a broom or vacuum to clean potentially contaminated areas as it can make the disease airborne.
How are hantaviruses maintained in nature?
Hantaviruses are maintained in nature in wild rodents. In California, mainly deer mice carry and shed SNV. Other rodents such as squirrels, chipmunks, and house mice are rarely, if ever, infected and do not pose a risk of HCPS to humans.
How is HCPS diagnosed?
Persons with HCPS can be readily diagnosed by specific blood tests. The problem lies in it frequently being misdiagnosed as common cold or flu.
For those who frequently handle or are frequently exposed to rodents in rural areas (such as mammalogists and pest control workers), CDC recommends wearing either a half-mask air-purifying (or negative-pressure) respirator or a powered air-purifying respirator (PAPR) with N-100 filters.
CDC does not recommend routine use of respirators by farmers and homeowners in rural areas. CDC guidelines (MMWR 1993; 42, RR-11) address specific risk-reduction measures for rural residents (rodentproofing, environmental management, and trapping) and precautions to be taken during activities that may pose increased risk of hantavirus infection (cleanup of rodent infested areas). Cleanup of very heavy rodent infestations or of homes associated with known cases of HPS are special instances for which we do recommend respiratory protection, and these tasks are best left to pest control or public health professionals. There is no evidence that farmers operating farm machinery in open fields (even though rodents may be crushed in the machinery) are at increased risk. Under these conditions, the natural circulation of air and virucidal properties of natural UV light make inhalation of infectious aerosols less likely. The possibility of human exposure is greater in indoor closed spaces, such as barns and sheds, that may be infested with rodents. It is important that outbuildings be rodent-proofed to the greatest extent possible. When effective rodentproofing is not possible, snap traps (and, if necessary, rodenticides) should be used continuously, and recommended precautions (concerning airing out and cleanup of infestations) should be followed when entering such buildings after periods of non-use.
What’s The Differences Between House Mice & Deer Mice?
Deer mice are similar in size to house mice but unlike the house mice, are grey to brown on top and white underneath, and have large unfurred ears. House mice tend to live inside and deer mice tend to live outdoors.